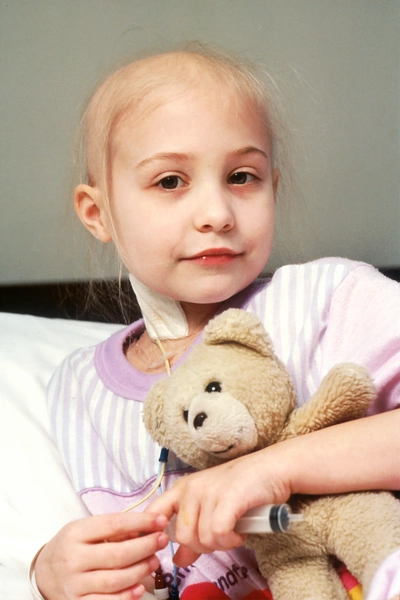
While the diagnosis of DIPG is difficult, there are steps you can take to improve the quality of care for your child.
DIPG is a type of tumor that starts in the brain stem, the part of the brain just above the back of the neck and connected to the spine. The brain stem controls breathing, heart rate, and the nerves and muscles that help us see, hear, walk, talk and eat. These tumors are called gliomas because they grow from glial cells, supportive cells in the brain.
About 10% to 20% of all childhood brain tumors are DIPG or brainstem gliomas.
They are more common in children between the ages of 5 and 10 years but can occur at any age in childhood. Though rare, they can also occur in adults.